BMI: Definitions & Measurement
by ACTION
How do we measure obesity?
The most common metric used for assessing the prevalence of obesity is the body mass index (BMI) scale.
The metric for measuring bodyweight in children and adolescents is also the body mass index (BMI) scale, measured in the same way described above. However, interpretation of BMI scores is treated differently for children and adolescents.
How do we measure obesity in adults?
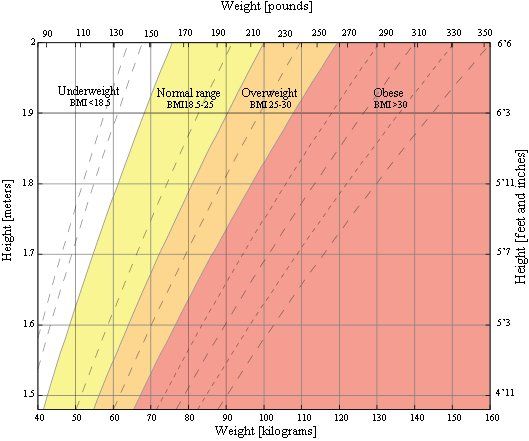
The most common metric used for assessing the prevalence of obesity is the body mass index (BMI) scale. The World Health Organisation define BMI as: “a simple index of weight-for-height that is commonly used to classify underweight, overweight and obesity in adults. It is defined as the weight in kilograms divided by the square of the height in metres (kg/m2). For example, an adult who weighs 70kg and whose height is 1.75m will have a BMI of 22.9.”
Measured BMI values are used to define whether an individual is considered to be underweight, healthy, overweight or obese. The WHO defines these categories using the cut-off points in the table. For example, an individual with a BMI between 25.0 and 30.0 is considered to be ‘overweight’; a BMI greater than 30.0 is defined as ‘obese’.
How do we measure obesity in children and adolescents?
The metric for measuring bodyweight in children and adolescents is also the body mass index (BMI) scale, measured in the same way described above. However, interpretation of BMI scores is treated differently for children and adolescents. Whilst there is no differentiation of weight categories in adults based on sex or age, these are important factors in the body composition of children. Factors such as age, gender and sexual maturation affect the BMI of younger individuals. For interpretation of individuals between the ages of 2 and 20 years old, BMI is measured relative to peers of the same age and gender, with weight classifications judged as shown in the table.
The merits of using BMI as an indicator of body fat and obesity are still contested. A key contention to the use of BMI indicators is that it provides a measure of body mass/weight rather than providing a direct measure of body fat. Whilst physicians continue to use BMI as a general indicator of weight-related health risks, there are some cases where its use should be considered more carefully14:
- muscle mass can increase bodyweight; this means athletes or individuals with a high muscle mass percentage can be deemed overweight on the BMI scale, even if they have a low or healthy body fat percentage;
- muscle and bone density tends to decline as we get older; this means that an older individual may have a higher percentage body fat than a younger individual with the same BMI;
- women tend to have a higher body fat percentage than men for a given BMI.
Physicians must therefore evaluate BMI results carefully on a individual basis. Despite outlier cases where BMI is an inappropriate indicator of body fat, its use provides a reasonable measure of the risk of weight-related health factors across most individuals across the general population.
BMI, formerly called the Quetelet index, is a measure for indicating nutritional status in adults. It is defined as a person’s weight in kilograms divided by the square of the person’s height in metres (kg/m2). For example, an adult who weighs 70 kg and whose height is 1.75 m will have a BMI of 22.9.
70 (kg)/1.752 (m2) = 22.9 BMI
For adults over 20 years old, BMI falls into one of the following categories.
Nutritional status
| BMI | Nutritional status |
|---|---|
| Below 18.5 | Underweight |
| 18.5–24.9 | Normal weight |
| 25.0–29.9 | Pre-obesity |
| 30.0–34.9 | Obesity class I |
| 35.0–39.9 | Obesity class II |
| Above 40 | Obesity class III |
More about Obesity & Resent Articles and Events

Obesity rates are rapidly increasing in the African Region, as in most parts of the world.
There is a common misconception that obesity and other noncommunicable diseases (NCDs) only occur among the wealthy.
Strategy for the prevention and control of Obesity in South Africa - 2015 - 2020
Act today for a healthier future. HSF supports the World Obesity Federation (WOF) in the initiative to stimulate and support practical actions to address obesity.
ACTION
African Centre for Obesity Prevention
PARTNERS
Join our growing list of partners, including:
Preventing obesity for a healthier tomorrow
Business Hours
- Mon - Fri
- -
- Sat - Sun
- Closed
About Us
Contact
Office:
+27 10 447 3721
E-mail: